|
|
||
|
Advance for Respiratory Care Practitioners, Vol 8, No 33, Aug 17, 1992; p 11.
How to Avoid the Intubation Blues
Desmond Allen, PhD, ND, RCP
|
||
|
Through the years I have often wondered why so many therapists and physicians have so much trouble performing even routine endotracheal intubations. Do they have a misunderstanding of anatomy? Could it be nerves? A lack of confidence? The inability to perform under pressure? Poor vision? Poor motor skills? What is the problem? I reality I know that none of these is the cause; at least not the primary cause. These people know the anatomy as well as I do. I have seen them work under pressure. They are confident, and their vision and motor skills are fine. I don’t mean to should like I never have trouble with an intubation. I do. But it is not often, and each troublesome intubation has its particular cause: excessive blood due to trauma, a short stout neck with such an anterior glottic opening that you never really see it clearly, a crying infant with a slimy NG tube in place. However, for the most part the great majority of my countless intubations over nearly 18 years have been routine. Furthermore, I must presume that my experience serves as a good cross section and, thus, a fait representation of the types of intubations and trouble encountered by others. “So,” I’ve wondered aloud, “Why the problem?” Then one day it struck me. I was staring into the throat of an infant no more than a few weeks old. The physician had elected to intubate him due to his progressive exasperation. I had a clear view of the glottis and had the tube camped out about a centimeter above it, ready for quick insertion. The baby was crying and the glottis was virtually closed, opening only occasionally and momentarily on inspiration (for which I patiently awaited). I thought to myself, “If I were looking only for what was taught in school, I would never get the tube in.” Students are taught to look for the vocal cords. Oh, the glottis is mentioned, but the emphasis is on the cords. But I new I wasn’t about to see the cords. My only landmark was the glottis, which now resembled a tiny mouth doing pursed lip breathing. Occasionally it would fly open for a slit second only to slam shut just as quickly. That brief moment during inspiration would be my chance to insert the tube. As I later reflected on this typical scene I realized that through the years many of the intubations I have performed were such that I had never seen the vocal cord. When a patient is in full arrest the cords are easily seen; but if a patient is still making any respiratory effort at all, the chances of seeing the cords are nil. Indeed, the greater the level of respiratory effort, the greater the likelihood of not seeing the cords. I began asking other what they were taught to look for during an intubation. In my search I questioned nurses, physicians, respiratory therapists and EMTs. Everyone had the same response: “The vocal cords.” “Could it be,” I thought, “that something so basic has been overlooked in all of our training?” Yes, it could be, I decided. Below I have listed some pointers that may help RCPs achieve a greater number of successful intubations.
1. Use the curved (Mac) blade for long necks and the straight (Miller) blade for short stout necks.
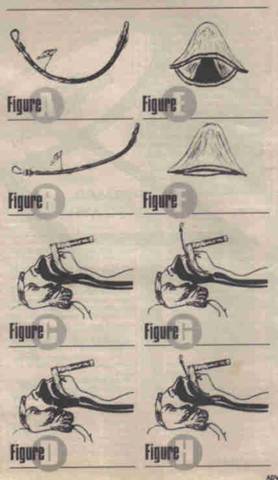
2. Don’t use the stylet to bow the tube too excessively (see figure A). A slight curve in the tube is often necessary for structural support in the event that you have to direct the tip of the tube upwards behind the epiglottis. However, your line of sight is direct; and to try to insert a tube that is markedly bowed can be awkward. Therefore I prefer a gentle bow throughout the length of the tube with a more prominent curve upward at just about the cuff level (see figure B).
The gentle bow provides structural support and the more prominent curve near the end of the tube allows you to advance the tip upward behind the epiglottis in the event that you cannot see the glottic clearly, much less the cords.
3. Hold the tube to the right of the laryngoscope blade. Don’t try to feed the tube through the curve on the blade. That will only obscure your vision of the glottis. New disposable blades don’t have this useless channel.
4. Look for the glottic opening, not the vocal cords. If you happen to see the cords, great! But don’t expect them. Besides, the cords are inside, just behind the glottic opening. Look for it. The glottis may be wide open (see figures C and E), in which case the cords may be seen.
However, if the patient is exhaling, the glottic opening will be nearly closed (see figures D and F). If so, it will resemble a tiny mouth doing pursed lip breathing. The two lips will be stretched taut with a minimal opening (see figure F). Wait for them to open on inhalation and then advance the tube (see figures G and H). Remember the average I/E ratio is about 2 or 3 to 1; and a situation with a depressed RR is even longer. Be patient for the glottis to open.
5. If you are unable to see beyond the epiglottis to view the glottic opening, place the tube just under and behind the epiglottis. Actually lifting it a bit (see figure G). Wait for the patient to inhale; then advance the tube (se figure H). You can listen through the tube for the breath. Once the tube as entered the glottic opening you will be able to hear the exhalations.
6. Don’t feel rushed. The suggested 30 seconds for completion is a long time.
Nasal Intubations 1. Begin to pass the tube like you would a nasal trumpet or a NT suction catheter. Once you are past the second obstruction stop.
2. Place your ear to the tube and listen for the breaths. Simply follow the inspirations. Stop advancing the tube as the patient’s inspiration ceases (for at this point the glottis is taut and all but closed on exhalation). When inspiration resumes, advance the tube again. If the patient begins to cough advance the tube rapidly as you would a NT suction catheter.
|